 A Sinhala word for this condition is yet to be coined which would be helpful to patients - Dr Galaboda
A Sinhala word for this condition is yet to be coined which would be helpful to patients - Dr Galaboda
It is a disease that has baffled many and little understood by the public at large. Characterised by cessation of breathing due to obstruction of the upper airways during sleep, it affects both, children and adults alike, causing serious health impacts. However, it is eminently preventable with some lifestyle modifications and early detection. During the past few years, the availability of diagnostic facilities have increased and are available at many government hospitals.
These diagnostic studies are comparable to world standards, says, Dr Thushara Galaboda , a Consultant Respiratory Physician at the District General Hospital, Hambantota, who has a special interest in the subject .
Following are excerpts of his interview with the Sunday Observer.
Q. Obstructive Sleep Apnoea is a little understood ailment. What causes it?
A. Obstructive Sleep Apnoea(OSA) is a disease characterized by cessation of breathing (apnoea) due to an obstruction of the upper airway during sleep. These patients develop obstruction of upper airway intermittently during deep sleep, which causes arousals from sleep and poses a variety of negative implications on their health as a whole.
 Q. Is it a serious condition? Does it affect adults and children?
Q. Is it a serious condition? Does it affect adults and children?
A. It can be a serious problem if the patient is affected severely. It can cause a variety of health as well as, social implications. It can affect both adults and children, but is commoner in adults.
Low quality fragmented sleep will not only cause excessive daytime sleepiness preventing maximum output , but put patients at high risk to developing cardiovascular diseases, including, heart attacks, high blood pressure, strokes, Diabetes, cardiac arrhythmias and sudden deaths during sleep.
Q. What happens to your body in Obstructive Sleep Apnoea?
A. When somebody is fast asleep, especially, if that person is obese, the upper airway becomes narrow gradually, which results in slowing down the airflow and sometimes total cessation of airflow. This limitation of airflow results in a transient drop in blood oxygen levels which ends with an arousal from the sleep.
He/she starts to breathe normally again and goes back to deep sleep. This cycle of events occurs repeatedly throughout the night. As a result he/she gets repeated episodes of low blood oxygen during sleep followed by arousals which will definitely lead to many health problems.
Furthermore, the individual gets low quality fragmented sleep which will cause excessive daytime sleepiness.
Q. Is it the same thing as snoring?
A. No, it is not the same. Snoring is a common occurrence during sleep and it is not a disease. However, some snorers can evolve into obstructive Sleep Apnoea. Almost all OSA patients snore. A snorer who has excessive daytime sleepiness may have this disease.
Q. What are the health impacts of Sleep Apnoea?
A. There are many serious health impacts. These patients have a high risk of developing cardiovascular diseases, including, heart attacks, high blood pressure, strokes, Diabetes Mellitus, cardiac arrhythmias and sudden deaths during sleep. Furthermore, as a result of excessive daytime somnolence, they are more prone to road traffic accidents and their work performance deteriorates. There may be relationship problems with the partner due to loud snoring.
 Q. Does sleepwalking have anything to do with Sleep Apnoea?
Q. Does sleepwalking have anything to do with Sleep Apnoea?
A. Sleepwalking is not a feature of sleep apnoea. Sleepwalking can occur due to other complex sleep disorder such as, parasomnias which can come with excessive daytime somnolence.
Q. What are the symptoms?
A. Excessive daytime sleepiness despite adequate sleep and snoring are the commonest presenting symptoms. They feel unrefreshed on waking up and sometimes experience choking episodes during sleep.
The bed partner sometimes witnesses cessation of breathing for some time( 10-20 seconds) during sleep. Other symptoms are, the need to pass urine several times during night, morning headache and poor memory and concentration.
Some patients have general malaise, lethargy and body weakness. A significant number of patients can come with complications of longstanding disease, such as, pulmonary hypertension( Raised pressures in lung vasculature and right heart) and heart failure.
Q. If detected early can it be prevented?
A. If this disease is detected early it can be treated easily, sometimes with lifestyle modifications and minor interventions. But, the important thing is to identify people with high risk for developing OSA and take necessary steps to prevent the development of OSA. Obesity is the single most important risk factor for OSA. Male gender, diabetes, are other risk factors.
Q. How is it diagnosed?
A. Suspected patients should undergo a sleep study which is called a polysomnography. Patients are monitored during sleep with the use of a sleep screening device.
That will record the breathing related parameters throughout the sleep which includes, changes in oxygen saturation, nasal air flow, snoring, pulse rate, etc. Some devices record EEG( electrical activity in brain), eye movements and muscle tone as well, in addition to respiratory parameters which is called a full polysomnography.
Depending on the number of obstructive events during sleep, based on polysomnography, OSA could be categorized to mild, moderate and severe disease.
The patient has to sleep in a room in the hospital which is called a sleep lab. But nowadays, especially, in western countries sleep studies are being done at home as it will give the true picture rather than sleeping in an unfamiliar set up.
Q. Is it curable? Treatable? Or is it a lifelong condition?
A. Mild cases could be cured with weight reduction and lifestyle modification. Severe cases are usually not curable unless he/she achieves significant weight reduction.
However, significant OSA is treatable successfully with a remarkable response. OSA due to a secondary cause such as enlarged tonsils can be cured by surgeries.
Q. How many identified patients do we have with this condition 1) globally 2) Sri Lanka?
A. This disease is increasingly recognized by the public and it is estimated that the prevalence of OSA in the US is 14% of men and 5% among women. Prevalence will continue to increase with the current epidemic of obesity.
The prevalence of OSA in Sri Lanka is largely unknown, mainly because of lack of awareness among the public, as well as, among the health professionals, and lack of diagnostic facilities. With the recent advancement in diagnostic facilities in Sri Lanka, it is increasingly diagnosed. Around fifty patients with OSA were diagnosed during the last 1 year duration in the District of Hambantota.
Q. What is the usual treatment procedure?
A. Treatment depends on the severity of the disease and the presence of symptoms. All patients who are obese need to reduce their weight. Smoking and alcohol are known to aggravate the condition and therefore should be avoided.
These patients should not use sedatives unnecessarily. Patients with moderate and severe disease who are symptomatic need to start CPAP (Continuous Positive Airway Pressure) treatment which is the definitive treatment, in addition to the lifestyle modifications I mentioned earlier.
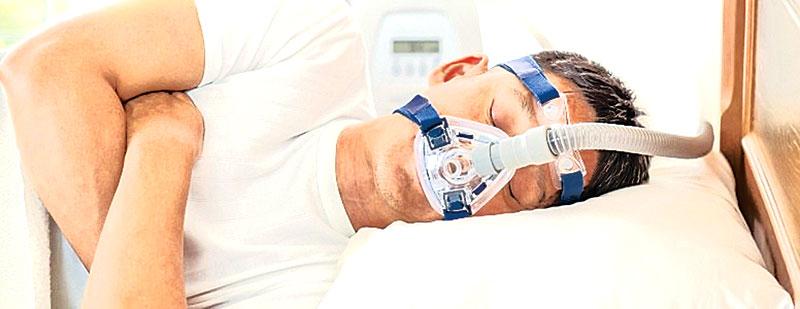
This is done usually after the exclusion of secondary causes of the upper airway obstruction by the help of the ENT surgeon. CPAP is a mask which the patient needs to wear during sleep and it covers in most instances, the mouth and the nose. It is connected to a small device via tubing and a pressure is applied to the upper airway to splint open the upper airway, so that part of the airway which tends to collapse during sleep is kept open throughout the sleep, preventing intermittent obstruction.
Q. Can everyone tolerate this procedure? If not, what is the alternative?
A. Some will not tolerate the mask and have the option of having surgeries in the throat. However, it may not be as effective as CPAP.
Q. What about patients with mild symptoms? Do they require surgery?
A. Patients with mild disease who are symptomatic may be benefited by oral splints( Mandibular advancement devices). It has shown that CPAP treatment is the most effective treatment for them. However, if they have upper airway obstruction due to a secondary cause e.g. enlarged tonsils, surgery is the treatment. Surgery may be beneficial in patients who cannot tolerate the CPAP mask.
Q. Are the facilities available here adequate? How well do they compare with world standards?
A. Diagnostic facilities were very limited until recent times .However, with the advancement of the field of pulmonology in Sri Lanka during last few years availability of diagnostic facilities have increased.
At present, it is available at many government hospitals, including, the National Hospital for Respiratory Diseases at Welisara, National Hospital of Sri Lanka, General Hospital Hambantota and Polonnaruwa, Teaching Hospitals in Kandy, Batticaloa and Jaffna. These sleep studies are comparable to world standards.
Q. Do we have enough specialists qualified in this field? Can a general physician be able to identify the symptoms and treat these patients?
A. Pulmonologists are the experts on this field and they are available in most major hospitals now. The Ministry of Health has been very helpful in providing them and they will be available in all hospitals with pulmonologists in the future. General practitioners and other specialists should be able to suspect the disease and refer the patient to a respiratory physician to perform a sleep study and start treatment, if needed.
Q. What are the present difficulties or gaps you see in the delivery of optimal care for such patients?
A. Lack of awareness of the disease among the public as well as the health professionals is a major drawback to identify the disease. A Sinhalese word for this illness has yet to be coined which will be helpful to create awareness among the public. Still the availability of diagnostic facilities is not up to standard and need to be increased in numbers. At present, the CPAP which is the definitive treatment is not given free by the government and it is expensive, which prevents most patients initiating treatment with CPAP. Oral splints used to treat milder cases are also not widely available at the moment.
Q. Can pre conditions like respiratory disease, asthma, cardiac problems, diabetes etc compound the disease?
A. Diabetes, obesity, some cardiac problems, certain respiratory diseases are risk factors for OSA. Untreated OSA can predispose to diabetes, strokes, high blood pressure and cardiac arrhythmias.
Q. What can be done to help these patients?
A. These patients need to be educated about the disease. Sleeping with a face mask may feel unusual in the initial days of treatment.
But, with the improvement of symptoms of daytime sleepiness, snoring, etc, they will realize the necessity and later on will not sleep without CPAP. The caregivers and the relatives also should be educated and they should support the patient to carry on with the treatment.
Q. Your message to the public?
A. As obesity is the single most important risk factor for OSA, all efforts should be taken to maintain an optimal weight by adopting a healthy lifestyle with balanced diet and regular exercises .
If somebody is a loud snorer and have excessive daytime sleepiness, he/she should be assessed further. Suspected patients need to be referred to a respiratory unit where facilities to do sleep studies are available.
