Multidisciplinary clinical teams across the world came together to pool their resources and share their knowledge on improving and strengthening care for Thalassaemia patients.
Multidisciplinary clinical teams across the world came together to pool their resources and share their knowledge on improving and strengthening care for Thalassaemia patients.
The Sunday Observer spoke to Dr. Manel Rathnayake, Consultant Haematologist, National Thalassaemia Center,Teaching Hospital, Kurunegala with inputs from the Director of the National Blood Transfusion Service, Dr Lakshman Edirisinghe and Consultant Paediatrician and Incharge of the National Thalassemia Centre, Teaching Hospital KurunegalaDr RanjaniEdirisooriya, to find out more about this condition which is reportedly on the rise in Sri Lanka .
Following are excerpts.
Q: World thalassaemia Day was observed on May 8. Why is a special day set aside for this particular health issue amid other pressing health problems?
A: The International Thalassaemia day was declared, to increase awareness amongst the general public about Thalassemia, with the aim of promoting and strengthening the care for these patients. The theme of this year is: “Empowering Lives, Embracing Progress: Equitable and Accessible Thalassaemia Treatment for All”.
Q: Can anyone get Thalassaemia?

Dr. Manel Rathnayake, Consultant Haematologist, National Thalassaemia Centre, Teaching Hospital, Kurunegala
A: Thalassaemia is an inherited genetic disorder of blood, leading to a condition known as anaemia. Haemoglobin is an important molecule in the red cells which carry oxygen throughout the human body. The production of the globin part of the haemoglobin molecule is controlled by a pair of genes received from both mother and the father. Depending on the genetic change, if one gene is genetically altered the result is Thalassaemia trait (thalassemia carrier state) while abnormality of both genes result in Thalassemia major. There are two types of globin chains in the haemoglobin molecule known as Alpha and Beta. According to the affected gene, Alpha or Beta thalassaemia trait Thalassaemia major can be diagnosed. In addition the structural changes of the globin chain will give rise to sickle cell disease, Haemoglobin E and D variants or combination of these leading to a Thalassaemia Intermedia state.
Q: Who are most at risk of developing this condition- age wise and gender wise?
A: Certain areas in Sri Lanka, particularly Kurunegala, Anuradhapura, Moneragala, Batticaloa and the Eastern coastal areas have increased prevalence of Thalassaemia carriers. Therefore, increased numbers of patients are seen in these areas. However, no district is free from Thalassaemia carrier state due to population migration.Because it follows an autosomal recessive mode of transmission, there is no gender-based differentiation among affected individuals.
Q: Can a pregnant woman transfer the thalassemia gene to her child during pregnancy?
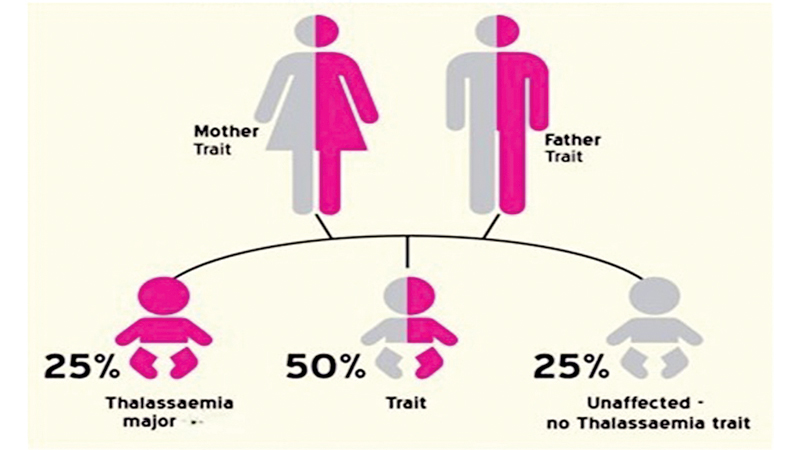
A: Genetic alteration and risk of becoming a thalassemia patient is dependent on both parents genetic makeup. If both parents are carriers, 25 percent of children can be Thalassaemia major patients, 50 percent can be Thalassaemia carriers and 25 percent can be normal. Thalassaemia carriers are asymptomatic. If only one parent is a carrier, 50% of children are carriers, while 50% of children can be normal. This is a probability and it is the same with each pregnancy.
Q: It has been reported that 3 in 100 of the world’s population have a thalassaemia gene. How many people in Sri Lanka suffer from this condition?
A: Thalassaemia carrier population is higher than 3 percent in some areas of Sri Lanka.According to recent statistics the number of thalassaemia patients is about 2000,with 60 new Thalassaemia patients born annually.
Q: What are the symptoms to watch out for in a person who may be carrying the gene?
A: Thalassemia carriers are asymptomatic with a subnormal haemoglobin level. The thalassemia patients will present within the first two years of life. The common symptoms are lethargy, poor feeding, and slow growth rate due to anaemia. A Pediatrician can confirm the diagnosis with clinical findings and laboratory tests.
Q: Do these symptoms vary from person to person – i.e. from mild to moderate to severe?
A: Yes.Transfusion Dependent Thalassaemiais due to Beta Thalassaemia major or severe form of E Beta Thalassaemia, which needs blood transfusions every 2-4 weeks to survive.
Less severe E Beta thalassemia and other compound heterozygous states may behave as mild or moderate severity and the frequency of blood transfusion is less hence categorised as Non-Transfusion Dependent Thalassaemia.
Q: In addition to anaemia, what are the main adverse impacts on the child?
A: Anaemia occurs invariably as there is ineffective red cell productionand premature breaking of red cells. The red cells will be produced in the liver and the spleen as well.
Therefore, these organs will enlarge significantly causing symptoms. If a patient is on an adequate regular blood transfusion program from the time of diagnosis, the enlargement of these organs will be suppressed.
The most devastating effects are due to iron overload of the body due to repeated blood transfusions. The human body does not have a way of eliminating excess iron. Each blood transfusion will add iron to the body stores and this iron can get deposited in the organs.
Most of the endocrine organs that produce hormones such as the pituitary, thyroid and pancreas can be affected in in addition to other main organs such as the heart, and liver.
If the iron overload is not removed satisfactorily by iron removing drugs, the patient eventually dies due to complications of iron overload such as heart failure, liver failure or by infections.
All these complications result in reduced life expectancy in patients.
Q: Can it result in bone deformities? If so, what are the most common sites?
A: Inadequate transfusion from early childhood results in expansion of the bone marrow space,which can be manifested in facial bones resulting in “thalassemia facies”.
Q: Can it affect the child’s development and growth? How?
A: They can suffer from hormone deficiencies due the damage caused by the iron deposition in hormone producing endocrine organs which may cause diabetes, thyroid dysfunction, impaired growth, development and secondary sexual development of a child.
Q: Treatment wise- what is the treatment given to reduce these symptoms? What does it involve? Walk us through the usual procedure?
A: A good transfusion regime and adequate iron chelation can minimise the complications. In addition, regular monitoring for complications and treatment is part of the management. They also have to bear painful needle pricks life long due to repeated blood testing, blood transfusions and for administration of parenteral iron chelating drugs.These can be minimised by curative treatments like Bone Marrow Transplant (BMT). Newer drug therapy(Luspatercept) and gene therapy are available in resource rich countries and can make the patient transfusion free.
Q: What is the best alternative to blood transfusion and other methods you referred to ? I understand that one of the most effective methods is by replacing the defective gene WITH a healthy donor marrow transplant? Do you agree? Why?
A: Yes. A successful bone marrow transplant can make a Thalassaemia patient ”cured” as he or she can be free from transfusion with the new set of genes producing adequate haemoglobin, minimising long term transfusion related complications.
Q: The theme for this year’s Thalassemia Day was “Empowering lives; Embracing progress: Equitable and Accessible Thalassemia treatment for all” What are the recent interventions that the Sri Lanka College of Haematologists has done to make this goal a reality? Dos and Don’ts?
A: The BMT team, led by the ConsultantHaematologist,is carrying out successful BMT for Thalassemia patients at Lady Ridgeway hospital and at major private hospitals. The procedure is complex and needs selection of appropriate patients with suitable matching donors.
The number of patients undergoing the BMT is limited due to various reasons including the unavailability of adequate space at the LRH, financial constraints and the unavailability of donors.
It should be appreciated that the government has allocated a significant amount of the health budget on developing a few centers for the BMT in the country.
However, in parallel establishing a stem cell donor registry to find donors among the community for BMT is also a crucial requirement which will take a few years to complete.
Once adequate number of donors are recruited to the registry, it would support the initiation of successful BMTs in the country with the completion of the infrastructure of the other BMT units.
The estimated cost of managing one Thalassaemia major patient is approximately USD 2602 annually as per the recent statistics. The cost benefit ratio is favorable on performing a BMT of a thalassaemia patient and making him or her transfusion free for the rest of their lives.
Q: Given the advances in this hi tech age, what is your prognosis for patients ensuring quality and accessible care for all Lankan patients with this condition?
A: With successful establishment of the BMT in the country whoever will be eligible for BMT can be cured. So the quality of life is improved.
The patients who are not suitable for BMT need comprehensive care which includes the management of their psychological, financial and social issues as well.
Q: Do you have a message for our readers out there?
A: Thalassaemia needs a multi-disciplinary and multisectorial approach involving the Haematologists, Paediatricians, Physicians and Transfusion Specialists, the community health care providers together with the Ministry of Health, re-implementing national health program for curative and preventive aspects of the disease. One of the most important aspects are improving public awareness of the disease and encouraging the young generation in the premarital age to understand the concept that the Thalassaemia patient’s births can be prevented if they make an intelligent decision by selecting the correct partner before their marriage.
The good primary health care system in Sri Lanka and the high literacy rate in the county provide ample opportunities to take measures for preventive strategies. In addition, the social media platforms that the youth are dealing with today with their mobile phones are one of the ideal ways to increase awareness.
Although not compulsory, re-emphasising the message through the marriage registrar’s offices by making thalassemia screening a requirement before registering a marriage will allow room for receiving information about their thalassemia status. This will not violate their right of selecting the partner but they are being informed about the risk of transmission of Thalassaemia well ahead before conception of a baby.Everyone is advised to get their thalassemia status known before the marriage.
A school thalassemia screening program is coordinated by the NCD unit of the Ministry of Health for grade 10 and above students. According to their diagnosis the different coloured cards are issued.A carrier is counselled and given a pink card while a confirmed non carrier will receive a green card with a green border. If a full blood count shows normal haemoglobin and red cell parameters, a green card with a yellow border is given without a confirmatory test.
The important message is that if both partners have green cards with a yellow border, that is a card without exclusion by a confirmatory test, one of the partners can undergo a confirmatory test before their marriage decision as rarely some Hb E thalassaemia carriers can have normal full blood counts. If one partner is excluded from a carrier state by a confirmatory test, there is no chance of getting a thalassemia major baby.
Such an arrangement has been advocated by the ministry of health of Sri Lanka as the cost for a confirmatory test is high and the economic situation will not permit to do the confirmatory test on each person.
Q: Is there a hotline they could contact if they wish to get more information?
A: The non-communicable disease unit of the Ministry of Health gives the leading role in organising programs for preventive strategies of Thalassemia in the country.
Any government hospital and community health care institutions in the country can provide information.
National Thalassemia centre in Kurunegala (Hotline 037 7917392) is open for services on weekdays from 8am to 4pm and Saturdays from 8am to 12noon.
When both parents are carriers, there is a 25 percent chance of giving birth to a Thalassaemia major baby. With each pregnancy the probability remains unchanged.