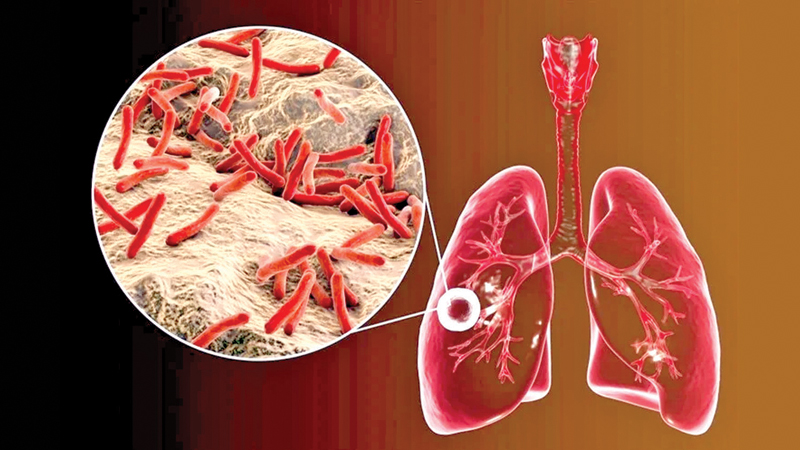
TB remains one of the world’s deadliest infections with thousands of persons dying or falling sick with complications each day across the world. Sadly it is the poorest and most overcrowded segments of the population that are the worst hit by this infectious yet largely preventable disease.
TB remains one of the world’s deadliest infections with thousands of persons dying or falling sick with complications each day across the world. Sadly it is the poorest and most overcrowded segments of the population that are the worst hit by this infectious yet largely preventable disease.
With the new government determined to make a change for the better, the Sunday Observer spoke to the Senior Registrar, National Hospital for Respiratory Diseases, Welisara Dr. Chanurdi Wickramathunga about the facts and myths surrounding TB and how we can drastically reduce the new cases being reported each day.
Excerpts
Q: What is TB?
A. Tuberculosis (TB) is a lethal disease caused by the bacterium Mycobacterium tuberculosis. It primarily affects the lungs but can also impact other parts of the body, such as the brain, kidneys, gut, skin and spine. TB is currently the world’s deadliest infectious disease.
Q: How is it spread?

Senior Registrar, National Hospital for Respiratory Diseases, Welisara Dr.Chanurdi Wickramathunga
A. TB is an airborne disease. It is spread by being exposed to respiratory droplets contained within the exhalations (coughs, sneezes, breath) of a person with active TB. TB can on rare occasions, pass from a mother to her baby during pregnancy (trans placental transmission)..
Q: Who are most at risk of getting it?
A. Prolonged exposure carries the highest risk. People living in close contact with someone with active TB such as healthcare workers, people in crowded settings (prisons, homeless shelters, refugee camps) are at high risk. Furthermore, there are several risk groups -people with weakened immune systems (e.g., HIV/AIDS, diabetes, cancer patients), malnourished individuals, alcohol addicts, elderly population and smokers.
Q: How is it diagnosed?
A. TB is diagnosed through clinical evaluation, medical history, and specific tests such as sputum smear microscopy, molecular tests, chest X-rays and culture of biological samples.
Sometimes even if your biological samples are not indicative of TB bacteria, your physician can decide to treat you as TB depending on the clinical evidence and imaging studies.
Q: What are the symptoms usually associated with TB?
A. The presentation varies depending on the organ system involved. If the lungs are involved, you can have persistent cough (lasting more than 2 weeks), fever and night sweats, unintentional weight loss, loss of appetite, fatigue, chest pain and difficulty breathing, coughing up blood (in severe cases.) If the vocal cords are involved, you will experience a voice change. If your gut is involved, you may experience long standing diarrhoea and sometimes distension of your stomach, and if your brain is involved there will be behavioral changes, and impaired consciousness.
Q: If I have cough for a few weeks, should I get tested for TB?
A. Absolutely. If you have a cough for more than 2 weeks, especially with fever or weight loss, you should get tested to rule out TB
Q: Can they be confused with any other disease which has similar symptoms at the start, like a viral flu?
A. Yes, TB can mimic many other diseases as well, leading to the risk of its neglect during the initial stage of the disease. And, there are instances where TB is incidentally diagnosed during routine medical checkups for medical certificates.
Q: Can TB be completely cured?
A. Absolutely! TB is completely curable with a full course of antibiotics taken for at least 6 months with proper follow-up. That is why it is important to detect it early and encourage patients to adhere to their treatment. However, the treatment duration may be extended in cases of multidrug-resistant TB (MDR-TB), depending on the system involved or if the patient defaults.
Q: What happens if someone stops taking TB medication early?
A. Stopping TB treatment early harms the patient as well as the wider community. It can lead to drug-resistant TB, which is harder to treat, and enables the infection to spread to other organs as well. Importantly, it endangers the defaulter’s families, and those who come in close contact with them.
Q: What is the DOTS method of testing TB?
A. The DOTS (Directly Observed Treatment, Short-course) strategy is not a test, but a treatment approach where trained personnel directly observe TB patients taking their medication to ensure adherence. As mentioned earlier, default has not just individual, but also social, ramifications.
Q: Is there a vaccine to prevent TB?
A. Yes, the BCG (Bacillus Calmette-Guérin) vaccine helps prevent severe TB in children but is not entirely effective in preventing pulmonary TB in adults. BCG provides only partial protection against adult pulmonary TB, and its efficacy can vary depending on geographical region, environmental factors, and individual immune responses.
Q: Can one continue working if he/she has TB?
A. That depends whether you are infectious or not. Usually, after sputum samples turn negative, which happens usually after two-weeks of adhered treatment, the patient is considered to be non-infectious. Until then, the patient must refrain from going to work. And even after the infection period, wear a mask when you are going to work.
Q: Can a person with TB travel by air?
A. No, you cannot travel by air until you become non-infectious, and your sputum samples test negative for TB bacteria. Since TB is an airborne disease, traveling in a confined space like an airplane poses a significant risk of spreading the infection to other passengers and crew members.
Once you start TB treatment, you usually become non-infectious after about two weeks, but this can vary depending on the severity of the disease and how well your body responds to medication. Before travelling, you should consult your doctor and get medical clearance to travel.
You must still take precautions to prevent exposing others to the bacteria, such as:
* Wearing a well-fitted mask (such as an N95) throughout your journey
* Covering your mouth and nose when coughing or sneezing to minimise the release of airborne bacteria
* Following your TB medication regimen strictly
If your TB is drug-resistant (MDR-TB or XDR-TB), more stringent travel restrictions may apply. Always check with your doctor and the airline’s policies before planning any travel.
Q: Are the myths that still prevail, a cause for delays in those with suspicious symptoms delaying seeing a doctor and be screened for TB?
A. Yes, definitely. Myths and misconceptions about TB contribute to delays in diagnosis and treatment, leading to increased transmission and worse health outcomes for those affected. Many people hesitate to seek medical help due to fear, misinformation, or social stigma. Some of the most common TB myths include:
* “Only poor people get TB.” – While TB is more prevalent in low-income communities due to factors like overcrowding, malnutrition, and limited healthcare access, anyone can get TB, regardless of economic status. Even wealthy individuals and professionals can be infected if exposed to the bacteria.
* “TB patients should be isolated permanently.” – People with active TB should take precautions, but after two weeks of proper treatment, most TB patients are no longer infectious. They do not need to be permanently isolated and can continue working or studying once their doctor confirms they are non-infectious.
* “TB is incurable.” – TB is completely curable with the correct treatment. Modern TB medications are highly effective when taken as prescribed. However, stopping treatment early or skipping doses can lead to drug-resistant TB, which is harder to treat.
* “If I feel better, I can stop taking TB medicine.” – Many patients stop taking TB medication once their symptoms improve, believing they are cured. This is dangerous because TB bacteria may still be present in the body, and stopping treatment too soon can lead to relapse and drug-resistant TB. A full course of TB treatment must be completed to fully eradicate the infection.
* “TB testing and treatment are expensive.” – In Sri Lanka, TB diagnosis and treatment are provided free of charge through government public health services, making it accessible to everyone.
Q: Can a person who had TB in the past get infected again?
A. Yes, a person who has had TB in the past can get infected again in two ways: reinfection and reactivation.
Reinfection occurs when the previously recovered patient is exposed to TB bacteria from an external source, they can develop TB again. This is more common in high-TB-burden areas, where people frequently come into contact with infected individuals.
Reactivation of Latent TB occurs if the immune system becomes weakened due to factors such as HIV/AIDS, diabetes, aging, malnutrition, cancer treatment, or long-term steroid use. The dormant bacteria can reactivate, leading to active TB disease.
Therefore, people who have recovered from TB should take precautions to prevent reinfection, such as avoiding prolonged close contact with active TB patients, maintaining a healthy immune system, and following up with healthcare providers if they develop any suspicious symptoms.
Q: Wasn’t TB eliminated from Sri Lanka some time ago?
A. No, TB has never been fully eliminated in Sri Lanka, and continues to be a major public health concern.
In 2022, 8,342 TB cases were reported in the country. However, WHO estimates indicate that the TB incidence rate was 62 per 100,000 population that year. Despite ongoing efforts, TB treatment coverage-which measures the proportion of reported cases compared to estimated cases—was only 60 percent, meaning that around 40 percent of TB cases remained undiagnosed or unreported.
Q: Does Sri Lanka have a goal for eliminating TB?
A. Yes, Sri Lanka has set a goal to reduce TB incidence from 65 per 100,000 in 2015 to 13 per 100,000 by 2035, demonstrating its commitment to eliminating tuberculosis, aligning with the WHO End TB Strategy. According to the WHO global tuberculosis report 2024 India (26 percent), Indonesia (10 percent), China (6.8 percent), the Philippines (6.8 percent) and Pakistan (6.3 percent) collectively account for 56 percent of the global TB burden. In comparison, Sri Lanka has a lower TB burden than many other South Asian countries.
Q: What do you see as the main challenges health officials face in this country with regard to achieving their set targets?
A. Several challenges hinder TB elimination efforts in Sri Lanka. Many cases go undetected due to stigma and fear of discrimination, discouraging individuals from seeking medical help. Additional factors such as overcrowded living conditions, poverty, illicit drug use, and a lack of social responsibility contribute to the persistence of the disease.
The rising incidence of the number of people living with HIVand multidrug-resistant TB (MDR-TB), particularly among individuals arriving from high-prevalence countries further complicates control efforts.
In 2023, 45.7 percent of Sri Lanka’s detected TB cases were reported from the Western Province, with Colombo District alone accounting for 24.6 percent. Other high-burden areas included Gampaha, Kalutara, and Kandy, highlighting the strong correlation between TB prevalence and high population density.
Q: What is your message to the public on how to protect themselves against TB?
A. I want to highlight a few points:
* Vaccination: Ensure children receive the BCG vaccine.
* Early detection: If you have a persistent cough for more than two weeks, seek medical help. If you know of anyone with symptoms, encourage them to undergo testing.
* Protect vulnerable people: People with weakened immunity should take extra precautions and proper control of glucose level if you have diabetes.
* Complete treatment: Follow the full TB treatment course to avoid drug resistance.
* Reduce the stigma: this is the most important thing – encourage people to get tested and treated without fear.